Guardians of a Continent
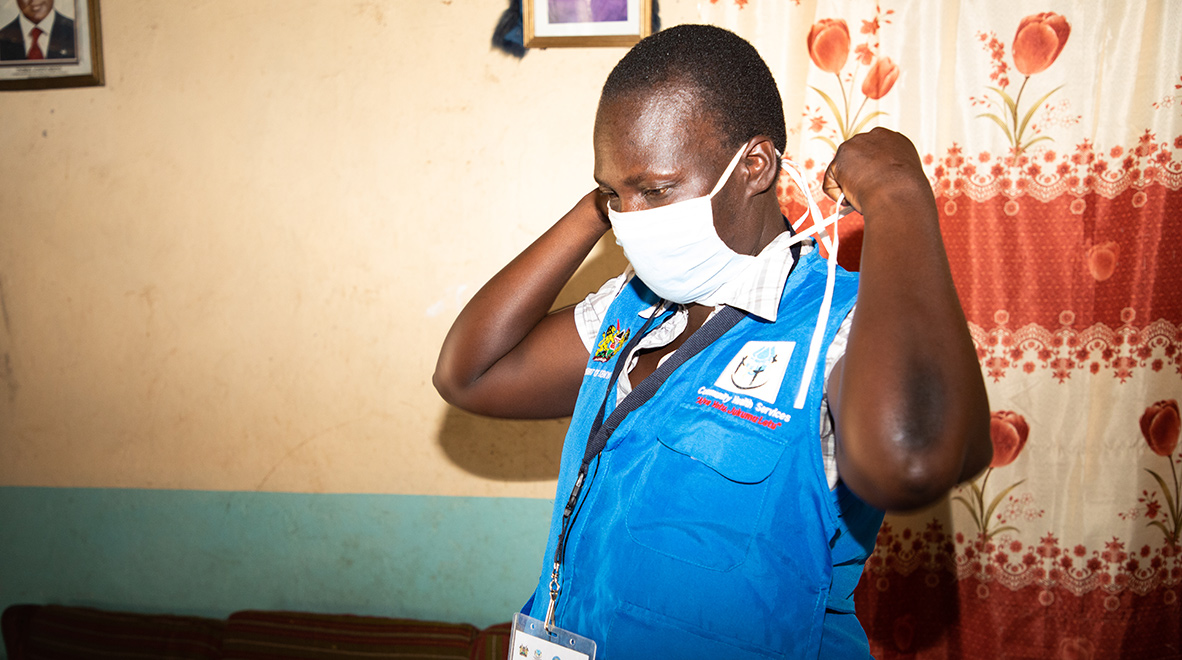
Every time Evaline Owuor says goodbye to her children and goes to work, she takes a calculated risk. As a community health worker in Kenya’s Homa Bay County, she has helped her community dramatically reduce the number of people who die from malaria. And when COVID-19 arrived, she enlisted to fight the new enemy.
But with limited personal protective equipment (PPE) such as masks and gloves, the worry of getting infected with the new virus is constant in Evaline’s mind. She knows she can be infected on the front lines – and potentially bring the virus home to her family – but she also knows she is needed to protect her community from the disease. COVID-19 can kill many people here as well as derail the great progress the community has made against malaria.
“Now that the new virus is here, I do two jobs,” Evaline says as she adjusts her mask. “In addition to malaria, I have to help my people dodge the new pandemic.”
COVID-19 collides with old epidemics
As COVID-19 accelerates in Africa, it is colliding with old epidemics and challenging public health officials to save lives while protecting massive gains made against other infectious diseases. Recent modelling studies from UNAIDS, WHO and the Stop TB Partnership show that the disruption to HIV, TB and malaria programs as a result of COVID-19 could lead to nearly a doubling of the number of deaths due to these diseases in just 12 months. We are already seeing this on the ground: The Global Fund’s biweekly survey of 106 countries shows the vast majority of HIV, TB and malaria service delivery has been disrupted.
The front lines have shifted
Behind the reception desk at Ogande dispensary – the health facility in Evaline’s home area – lead nurse Joan Got spoke of a drastic drop in the number of patients coming to see her. COVID-19, she says, has imbued the health facility with a cloud of stigma that makes many people afraid of visiting. As that mistrust in formal health facilities increases, community health workers are filling the gaps. The trust built over the years in the community by these grassroots health workers is critical to reach people in need with lifesaving tests, prevention and treatment. The challenge of fewer patients visiting health facilities has been reported far beyond this corner of western Kenya – in health facilities in Ghana and the Gambia, in Nigeria and Mali, in Sierra Leone and Senegal. Malaria program managers from these countries recently told an online webinar organized by the Global Fund that one of the most notable effects of COVID-19 in the provision of care and treatment for malaria is that the front lines have shifted – more than before, communities are putting their health firmly in the hands of community health workers.
Dr. Diwe Ekweremadu, a deputy chief of party with Catholic Relief Services in Nigeria, says visits by malaria patients to health facilities catering for internally displaced communities in northeastern Nigeria have plummeted – but at the same time, community health workers are testing and treating more people.
Across Africa, the crucial role community health workers play as guardians of community health has come into clear focus. Community health workers like Evaline have over the years led the fight against killers such as malaria, HIV and TB.
There are approximately one million community health workers in the countries where the Global Fund invests in Africa. These health workers – most of whom are volunteers getting small stipends to protect their communities from diseases – are now facing COVID-19 head on. To continue lifesaving support and avoid a catastrophic setback in the fight against HIV, TB and malaria, protecting them from harm is fundamental.
Social capital
Mary Okwaro, program manager at Kinda Women Group where Evaline works, recalls how far her community has come in the fight against infectious diseases in the past 25 years. “At the beginning, there was no treatment for HIV. We were using improvised solutions to try to keep people alive,” she recalls. “Those were tough days.”
There were also challenges of acceptance of community health workers by people working in formal health systems. Many didn’t believe community health workers could run accurate rapid diagnostic tests, for instance, says Patrick Igunza, a monitoring and evaluation official with Amref Health Africa, which supports more than 11,000 community health workers to fight TB and malaria in Kenya. But with time, these biases evaporated. Since 2016, for instance, the community health workers managing malaria under Amref Health Africa have conducted 1.4 million malaria tests in homes and treated 800,000 cases as well as supported malaria prevention. This work has helped send malaria in places like western Kenya into retreat.
Today, the health of millions of people in Africa’s rural areas is supported by the social capital and trust built around community health workers. African governments are looking to put these health workers firmly on the front lines of the new pandemic. The African Union has a new COVID-19 response fund that, among other things, aims to “support the deployment of one million community workers and community healthcare workers to support contact tracing” across the continent.
In South Africa, more than 30,000 of them have moved door to door, screening people and identifying the coronavirus infections before the people go to health care facilities. And as the pandemic surges in Kenya, the country has realized that it cannot accommodate all COVID-19 patients in hospitals, it has now turned to more than 63,000 community health workers to support home-based isolation and care operations for the pandemic.
Urgent need for protective gear
As community health workers take on the rising tide of COVID-19 in Africa, the stakes are high. Worries of escalating infections abound. The shortage of training and protective gear such as proper masks and gloves is dire, putting health workers at increased risk of infection and of unknowingly transmitting the disease to others.
In western Kenya, Evaline and her colleagues say they need more additional protective gear now, before the disease escalates and puts them, their families and community at greater risk. The current supplies Mary at Kinda Women Group and her colleagues have can barely meet the need. “We can defeat this pandemic if we have enough PPE,” says Mary. “Unfortunately, we are making do with little.”
Protecting front-line health workers is fundamental to mounting an effective response to COVID-19 and to continuing the fight against HIV, TB and malaria. The Global Fund is investing in protecting community health workers and other front-line health workers through provision of personal protective equipment. The Global Fund is seeking to invest more as it strives to see that all front-line health workers, including those serving in remote rural villages like Evaline, are protected from the coronavirus.
Resilient Systems for Health
Learn more